by Melissa Blake, ND
Immune resilience has never been more important or desired than in the past year. As a result of a global pandemic, patients and practitioners alike are seeking effective solutions to ensure a robust immune defense.
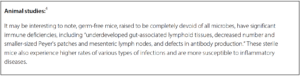
Outside of the current COVID-19 concerns, respiratory tract infections (RTIs) pose a significant burden and are, in children, elderly, and immunocompromised individuals, the most prevalent diseases globally.1
A well-balanced gut microbiota is associated with protection against various diseases, including respiratory infections, and the literature strongly supports an important clinical role for probiotic supplementation in promoting immune resilience and homeostasis.2
This article reviews the evidence for probiotics in the prevention and management of RTIs through their impact on the gut-lung microbiota axis.
| Clinical considerations:
The effective use of probiotics in immune protocols may be more nuanced than a one-size-fits-all approach. In an effort to support a personalized approach, outcomes of several strain-specific clinical trials are outlined in Table 3. |
The gut-lung microbiota axis
A significant portion of immune tissue resides with the gastrointestinal (GI) system and is constantly in contact with a wide variety of “nonself” molecules. The intestinal epithelial lining plays an essential role in our nonspecific immune response as a barrier against pathogens.2 Microbial communities within this environment begin shaping the immune system early on, with continued influence on its function and maintenance throughout one’s lifetime.2
Research on inflammatory lung diseases points to gut dysbiosis as a contributing cause and suggests an important connection between the gut microbiota and lung health.2
Interestingly, this relationship appears to be bidirectional, as alterations in the lungs also lead to changes in the gut.3,4
In fact, acute infectious and chronic inflammatory respiratory conditions consistently demonstrate both gastrointestinal symptomology and altered gut microbiota.3 From asthma to influenza, research is beginning to reveal the intimate, bidirectional relationship between the gastrointestinal and respiratory systems.1,3
Although the exact mechanisms are still unclear, it has been suggested that the intestinal microbiota can directly impact immune responses within the lungs by influencing the bacterial composition of the respiratory tract and through beneficial, immunomodulatory metabolites that can travel from the gut to the lungs.3
| Clinical considerations:
With the delicate balance and significant cross-talk that occurs along this gut-lung axis in mind, it seems prudent to support a balanced gut microbiota. Probiotics may offer an exciting option in respiratory infections, with the potential for fewer side effects and better outcomes. |
The consequence or the cause: addressing dysbiosis with probiotics
Dysbiosis is a disease-promoting imbalance in the composition of microbiota and can occur as the result of many factors (Table 1). A disrupted gut microbiota is a common feature associated with increased susceptibility and aggravations of a variety of disease states.2,6
Table 1: Intrinsic and environmental factors associated with dysbiosis2,3,5-7
Recent research links gut dysbiosis to disease severity in patients with COVID-19.8 Independent of treatment protocols, patients with confirmed infection had altered microbiota composition when compared to uninfected individuals.8 Dysbiosis also correlated with elevated levels of C-reactive protein (CRP), lactate dehydrogenase (LDH), aspartate aminotransferase (AAT), and gamma-glutamyl transfererase (GGT).8
Evidence suggests dysbiosis contributes to disease severity thru immune and proinflammatory pathways and that probiotic therapy may offer a solution by supporting a microbiome that is rich and diverse in commensal bacteria and stable and resistant to opportunistic ones.6,8 Through local and systemic pathways, probiotics promote an anti-inflammatory phenotype that supports immune resilience and homeostasis.3
Side note:
The possible mechanisms associated with probiotics are outlined in Table 2.
Table 2: Suggested mechanisms of action associated with probiotics1,4,9
| Clinical considerations:
Probiotic therapy may address dysbiosis, whether preexisting or the consequence of infection, and may encourage immune resilience as part of a preventative and a management strategy against respiratory infections. |
Probiotics: A role in prevention and management of respiratory tract infections
As indicated by several systematic reviews, substantial evidence exists to support probiotic therapy in the prevention and management of RTIs.10,11
Two separate meta-analyses suggest a 47% reduction in RTI incidence in probiotic groups compared to placebo, along with a shorter duration of RTIs by 1-2 days.12 These meta-analyses, however, do not separate results based on age or strain and excluded studies conducted in athletes.
Although the evidence is promising, what is lacking is an in-depth understanding of strain-specific benefits, and further research is needed to better understand impact, especially as it relates to patient demographics including age, sex, and ethnic background.
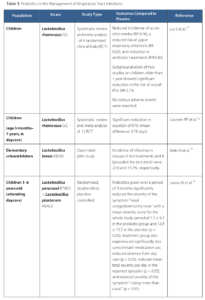
A high-level overview of strain-specific benefits of probiotics on RTIs is summarized in Table 3.
Table 3: Studies on strain-specific benefits of probiotics on RTI outcomes
| Clinical considerations:
A balanced gut microbiota is not only associated with immune resilience and homeostasis but with a wide variety of clinical benefits. These significant health-promoting properties, along with an impressive safety profile, make probiotics a powerful option to include in a clinical immune toolkit. |
Conclusion
So intimate is our relationship with the microbes we play host to that we do not simply benefit from their existing but are dependent on them as an essential part of human physiology.
Growing evidence reveals an important connection between gut health, including epithelial barrier integrity and microbial balance as well as susceptibility to and severity of respiratory infections.
Clinicians may want to consider the systemic impacts of probiotic supplementation via the gut-lung axis and the potential therapeutic benefits of probiotic therapy on immune resilience. Considering the current climate, along with substantial evidence to support their use, probiotic supplementation may be an essential therapeutic consideration in the prevention and management of a range of immune-related concerns, including respiratory tract infections.
Citations
- Din AU et al. SARS-CoV-2 microbiome dysbiosis linked disorders and possible probiotics role. Biomed Pharmacother. 2021;133:110947.
- Shahbazi R et al. Probiotics in treatment of viral respiratory infections and neuroinflammatory disorders. Molecules. 2020;25(21):4891.
- Marsland BJ et al. The gut-lung axis in respiratory disease. Ann Am Thorac Soc. 2015;12 Suppl 2:S150-156.
- Hanada S et al. Respiratory viral infection-induced microbiome alterations and secondary bacterial pneumonia. Front Immunol. 2018;9:2640.
- Weiss GA et al. Mechanisms and consequences of intestinal dysbiosis. Cell Mol Life Sci.2017;74:2959–2977.
- Dumas A et al. The role of the lung microbiota and the gut-lung axis in respiratory infectious diseases. Cell Microbiol. 2018;20(12):e12966.
- Levy M et al. Dysbiosis and the immune system. Nat Rev Immunol. 2017;17:219–232.
- Yeoh YK et al. Gut microbiota composition reflects disease severity and dysfunctional immune responses in patients with COVID-19. Published online January 2021.
- Science Review: Probiotic Research and Clinical Benefits. Metagenics Institute. Accessed January 11, 2021. https://www.metagenicsinstitute.com/ce-education/science-sheets/probiotic-benefits/
- Wang Y et al. Probiotics for prevention and treatment of respiratory tract infections in children: A systematic review and meta-analysis of randomized controlled trials. Medicine (Baltimore). 2016;95(31):e4509.
- Hao Q et al. Probiotics for preventing acute upper respiratory tract infections. Cochrane Database Syst Rev. 2015;(2):CD006895.
- Karl JP. Gut microbiota-targeted interventions for reducing the incidence, duration, and severity of respiratory tract infections in healthy non-elderly adults [published online ahead of print, 2020 Nov 2]. Mil Med. 2020;usaa261.
- Liu S et al. Lactobacillus rhamnosus GG supplementation for preventing respiratory infections in children: a meta-analysis of randomized, placebo-controlled trials. Ind Peds. 2013;50(4):377-381.
- Laursen RP et al. Probiotics for respiratory tract infections in children attending day care centers-a systematic review. Eur J Pediatr. 2018;177(7):979-994.
- Waki N et al. Effects of probiotic Lactobacillus brevis KB290 on incidence of influenza infection among schoolchildren: an open-label pilot study. Lett Appl Microbiol. 2014;59(6):565-571.
- Lazou AI et al. Evaluation of the efficacy of Lactobacillus plantarum HEAL9 and Lactobacillus paracasei 8700:2 on aspects of common cold infections in children attending day care: a randomised, double-blind, placebo-controlled clinical study. Eur J Nutr. 2020;59(1):409-417.
- Leyer GJ et al. Probiotic effects on cold and influenza-like symptom incidence and duration in children. 2009;124(2):e172-179.
- Berggren A et al. Randomised, double-blind and placebo-controlled study using new probiotic lactobacilli for strengthening the body immune defence against viral infections. Eur J Nutr. 2011;50(3):203-210.
- West NP et al. Probiotic supplementation for respiratory and gastrointestinal illness symptoms in healthy physically active individuals. Clin Nutr. 2014;33(4):581-587.
- Turner RB et al. Effect of probiotic on innate inflammatory response and viral shedding in experimental rhinovirus infection – a randomised controlled trial. Benef Microbes. 2017;8(2):207-215.
- Namba K et al. Effects of Bifidobacterium longumBB536 administration on influenza infection, influenza vaccine antibody titer, and cell-mediated immunity in the elderly. Biosc Biotech Biochem. 2010;74(5):939-945.
- Wang B et al. Probiotics to prevent respiratory infections in nursing homes: a pilot randomized controlled trial. J Am Geriatr Soc. 2018;66(7):1346-1352.
NCFM® and Bi-07® are registered trademarks licensed by DuPont.
Melissa Blake, ND is the Manager of Curriculum Development at Metagenics. Dr. Blake completed her pre-medical studies at Dalhousie University in Halifax, Nova Scotia and obtained her naturopathic medical training from the Canadian College of Naturopathic Medicine. Dr. Blake has over 10 years of clinical experience, specializing in the integrative and functional management of chronic diseases.