How Specific Strains of Lactobacilli and Bifidobacteria Work Together
Probiotics have a long history of safe1 and effective use, with clinical studies demonstrating strainspecific effects on specific conditions.2 The early identified probiotic Lactobacillus acidophilus NCFM® (L. acidophilus NCFM) has been used in foods and supplements since 19703 and has demonstrated clinical efficacy alone and even more so with other strains. Lactobacillus rhamnosus GG (L. rhamnosus GG) is one of the most widely studied lactobacilli, patented in 19894 and has been widely adopted for acute gastroenteritis in children.4–7 These strains as well as others highlighted here can work together in particular dose and strain combinations to impact gut microbiota, gastrointestinal (GI) function, and immune function.
Probiotics have a long history of safe1 and effective use, with clinical studies demonstrating strain-specific effects on specific conditions.2 The early identified probiotic Lactobacillus acidophilus NCFM® (L. acidophilus NCFM) has been used in foods and supplements since 19703 and has demonstrated clinical efficacy alone and even more so with other strains. Lactobacillus rhamnosus GG (L. rhamnosus GG) is one of the most widely studied lactobacilli, patented in 19894 and has been widely adopted for acute gastroenteritis in children.4–7 These strains as well as others highlighted here can work together in particular dose and strain combinations to impact gut microbiota, gastrointestinal (GI) function, and immune function.
Key mechanisms of action
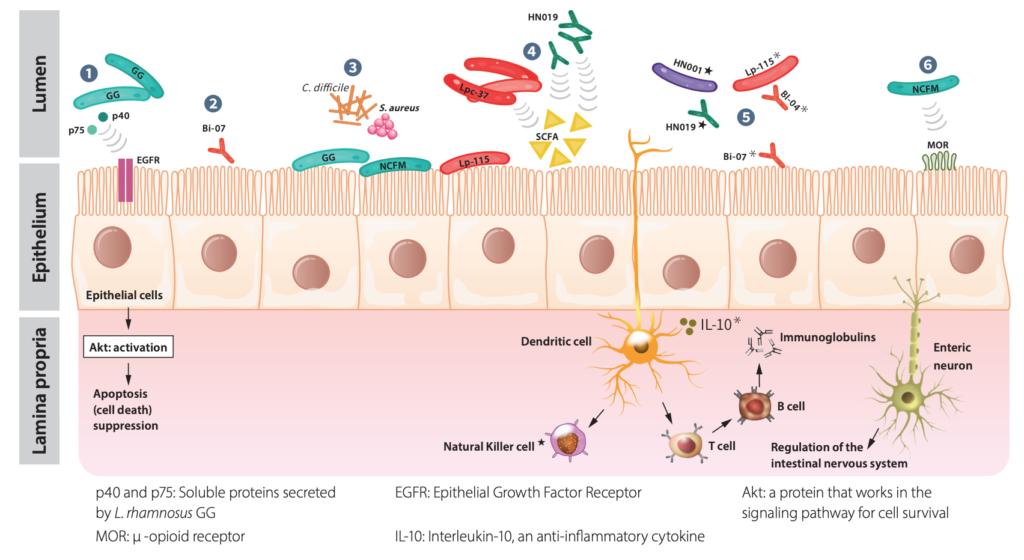
The mechanism of action of probiotics are complex and differ by strain. Mechanisms of action described below were determined through preclinical research unless otherwise indicated.
- Intestinal Barrier Support: Decrease in intestinal cell apoptosis by L. rhamnosus GG33-36
- Suppression of intestinal hyperpermeability: Mitigation of bacterial translocation, intestinal permeability increases, and inflammatory biomarker increase by B. lactis Bi-0737
- Inhibition of pathogenic microorganisms: C. difficile and Staphylococcus aureus may attach to intestinal epithelial cells and cell receptors; displacement of these pathogens by L. rhamnosus GG and L. acidophilus NCFM, L. plantarum Lp-11538
- Production of Useful Metabolites: Production of short-chain fatty acids (SCFA) in children’s feces by L. paracasei Lpc-37 or B. lactis HN01939 Lactobacilli and bifidobacteria produce lactate and acetate28,40
- Immune activity: Increase in the activity of natural killer cells in elderly humans by L. rhamnosus HN001 or B. lactis HN01917,19,41-42 Induction of secretion of anti-inflammatory cytokines by B. lactis Bl-04 and Bi-0743 Stimulation of immune response via increased immunoglobulins during vaccination in people by L. plantarum Lp-115 as well as B. lactis Bi-07 and Bl-0420
- Regulation of the intestinal nervous system: Regulates the expression and activity of intestinal opioid receptors in humans with abdominal pain: L. acidophilus NCFM44
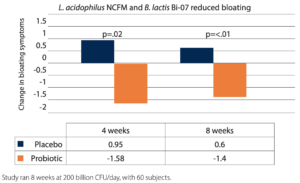
Bloating: In a double-blind, randomized, placebo-controlled trial (RCT), L. acidophilus NCFM® and Bifidobacterium animalis subspecies lactis Bi-07® (B. lactis Bi-07) reduced bloating symptoms by 15% in patients with functional bowel disorders (FBD).8
Pain post-colonoscopy:
In a RCT of 320 patients, 12.5 billion colony forming units (CFU) L. acidophilus NCFM and 12.5 billion CFU B. lactis Bi-07 per day for two weeks reduced pain time 28% (19 hours) for patients following colonoscopy, a significant change (p<.033).9
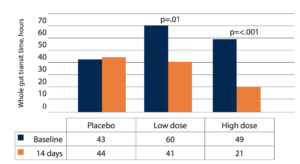
Constipation: In a RCT of 100 adults, a 30-50% reduction in whole gut transit time was achieved with 1.8 and 17.2 billion CFU Bifidobacterium animalis subspecies lactis HN019 (B. lactis HN019) as shown in the graph below. Consumption of B. lactis HN019 led to a reduction in constipation, irregularity, and flatulence about two times greater than the placebo.10
Flatulence:
When B. lactis HN019 was added to L. acidophilus NCFM, B. lactis Bi-07, Bifidobacterium animalis subspecies lactis Bl-04 (B. lactis Bi-04), and Lactobacillus paracasei Lpc-37 (L. paracasei Lpc-37) (the four-strain combination was cited by the World Gastroenterology Oraganisation’s Global 2017 guidelines for antibiotic-associated diarrhea7 ), the five-strain combination showed a statistically significant reduction in flatulence. In addition, less digestive discomfort was observed. The treatment included consumption of the combination for two weeks for a total of 156 constipated people in the RCT.11
Combining benefits: a novel, multi-strain formula
When combining multiple strains of probiotics for health benefits, even though each strain has a demonstrated health benefit and has been safely consumed, the combination may behave differently. The eight strains in these studies were combined together into a unique and novel combination. An IRB-approved clinical study on the combination resulted in no serious adverse events and no withdrawal of participants.
Stool testing showed that Lactobacillus species increased significantly and Bifidobacterium species also increased, but the change was not statistically significant. Unexpectedly, once-daily consumption over 10 days resulted in higher levels of Faecalibacterium prausnitzii (F. prausnitzii) and Akkermansia muciniphila. These findings were statistically significant, suggesting that the novel multi-strain combination impacts gut microbial composition.27
The possible mechanism may be that acetate produced by the lactobacilli28 and bifidobacteria29 may encourage the growth of Faecalibacterium prausnitzii. F. prausnitzii produces butyrate as a metabolite, which supports the growth of intestinal goblet cells, which produce mucin, a food source for Akkermansia muciniphila.30 These two cohabitants of the intestinal mucosa are lower in many disease conditions of the intestine associated with metabolism and inflammation.31, 32 Additional research on this novel multi-strain combination is warranted to evaluate published benefits on the strains as well as how these strains work together to provide additional benefits.
Antibiotic-associated diarrhea:
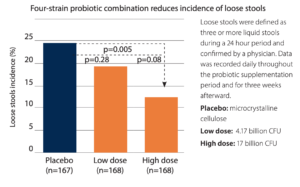
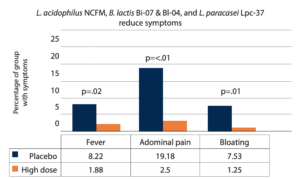
L. acidophilus NCFM, B. lactis Bi-07 and Bl-04, and L. paracasei Lpc-37 at 17 billion CFU reduced antibiotic-associated symptoms by more than 50% fewer days of diarrhea and more than 80% less bloating and abdominal pain in a large RCT. Clostridium difficile-associated diarrhea was significantly lower (p=0.02) comparing the high dose group to the placebo group. The capsule was taken two hours after the antibiotic and breakfast. Probiotic usage continued one week after the antibiotic course completed.12
Clostridium difficile:
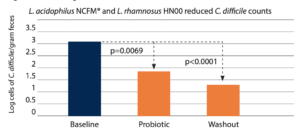
In a randomized crossover trial, L. acidophilus NCFM and Lactobacillus rhamnosus HN001 (L. rhamnosus HN001) eaten in cheese reduced Clostridium difficile as measured in feces of C. difficile-positive elderly after four weeks. An additional four weeks without the probiotic showed a continued reduction in C. difficile counts.13 This study was cited by the World Gastroenterology Organisation 2017 guidelines.7
Upper respiratory tract infections:
A meta-analysis of probiotics concluded that in general, probiotic use was associated with an 8% reduction in relative risk of developing a cold.14 In particular, 2 billion CFU B. lactis Bl-04 was found to reduce risk of a cold by 27% (with statistical significance), while the combination of L. acidophilus NCFM and B. lactis Bi-07 also reduced the risk (19%) compared to placebo in a RCT of healthy, active adults.15
Natural killer cell activity:
L. rhamnosus HN001 at 5 billion CFU/day increased cellular phagocytosis and natural killer cell activity in blood for healthy elderly who consumed it in milk for three weeks in two trials.16,17 B. lactis HN019 supported immune cell function in the elderly with an increase in natural killer cell activity, also at 5 billion CFU/day.16,18,19
Immune response:
Vaccination can be improved with adjuvants, which are additional components that may help stimulate the immune response to the offending compound (antigen). Probiotics have been tested in vitro for their ability to modify the immune system and therefore are potential candidates to help with improving the efficacy of vaccination. Measuring serum and salivary immunoglobulins may be an indicator of immune response. Specifically, IgG is involved in immune memory.
A study evaluated the changes in immunoglobulins, various proteins that act as antibodies in the immune system response, in blood as well as in saliva in response to one of seven probiotic strains (20 billion CFU each) or a placebo. In this eight-arm RCT using probiotic consumption over three weeks during two vaccinations, B. lactis Bl-04 was one of two strains that showed a significant change to serum IgG; Lactobacillus plantarum Lp-115 as well as B. lactis Bi-07 also increased serum IgG compared to placebo although the changes were not significant.20
Allergy, gut-skin axis:
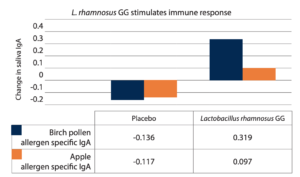
Some evidence has shown that L. rhamnosus GG demonstrated improved tolerance to milk in children with a milk allergy.21–23 In young adults with birch pollen and apple allergies, a RCT tested consumption of 20 billion CFU per day of L. rhamnosus GG for five and a half months during the birch pollen season. The probiotic-treated group was shown to stimulate secretion of birch pollen and apple-specific IgA.24 Increases in allergen-specific IgA levels suggest support for an immune response that tolerates the allergen.25
Stress, gut-brain axis:
In a randomized, double-blind placebo-controlled trial, 120 healthy adults between the ages of 18 and 25 consumed either the probiotic L. paracasei Lpc-37 or the placebo once daily for 5 weeks and took the Trier Social Stress Test (TSST) before and after the intervention. Participants who received Lpc-37 reported significantly lower perceived stress levels compared to the placebo group by the end of the study (p=0.048).26