Vitamin D
Vitamin D is an essential, fat-soluble vitamin that acts as a steroid hormone and plays a central role in many components of our skeletal and extraskeletal health. Vitamin D is naturally present in some fish, mushrooms, and eggs; in select fortified foods such as milk products; and also in the form of dietary supplements and pharmaceuticals. It is also synthesized in the skin from 7-dehydrocholesterol when exposed to ultraviolet B (UVB) rays from sunlight.1
| Download the PDF |
Research Highlights
- Vitamin D is important for calcium homeostasis, bone mineralization, and promoting immune and cardiovascular function1
- Vitamin K is important in blood coagulation, and plays a central role in decreasing calcium accumulation in the smooth muscles of vascular walls2
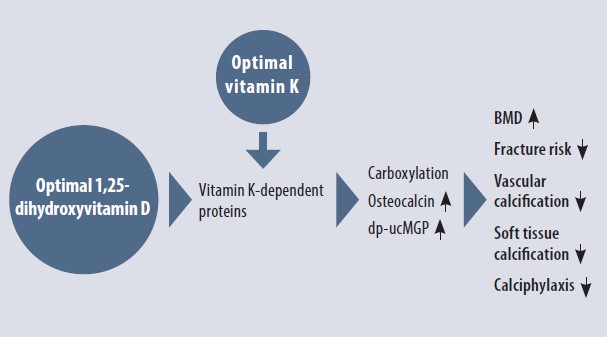
- Vitamins D and K have a synergistic relationship since vitamin D positively impacts the production of vitamin K-dependent bone proteins to induce bone formation and reduce vascular calcification3
There are two forms of vitamin D: D2 (ergocalciferol) obtained from plants, mushrooms, and yeast; and D3 (cholecalciferol) obtained from animal products such as fatty fish, fish liver oil, egg yolk, and beef liver.4
Vitamin D obtained from food, supplements, or sunlight is considered a preprohormone that is biologically inactive. It must undergo two separate hydroxylations in the body for the activation to occur and function as a hormone. The first hydroxylation occurs in the liver by the enzyme 25-hydroxylase where it is hydroxylated to form 25-hydroxyvitamin D (25(OH)D), or calcidiol.1,4-6 This is the major circulating form of vitamin D and is used as the clinical measure for serum vitamin D status. The second hydroxylation reaction occurs in the kidney by the enzyme 1-α-hydroxylase to form 1,25-dihydroxyvitamin D (1,25(OH)2D), or calcitriol, its active form.1,4-6 Vitamin D-binding protein transports vitamin D and its hydroxylated forms in the blood to target tissues.
Vitamin D in the Body
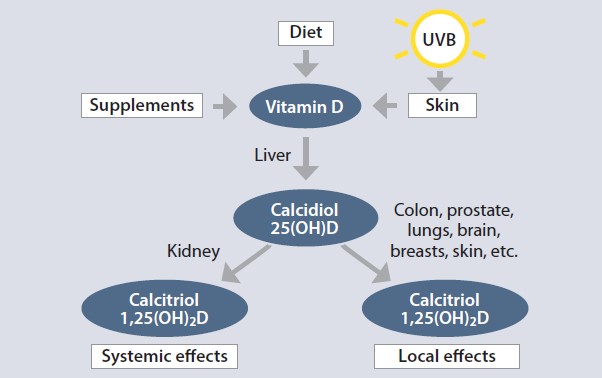
Functions of vitamin D
Vitamin D plays a major role in regulating calcium metabolism by increasing intestinal calcium absorption and maintaining adequate levels of calcium in the blood.5-6 It also maintains adequate phosphorus levels in the body, which together with calcium, aids in bone growth and remodeling as well as normal mineralization of bone.5-6 Along with these indirect effects on bone, the active form of vitamin D is involved directly in bone cell functions. Some extraskeletal functions of vitamin D include immune and cardiovascular function, reduction of inflammation, and modulation
of cell growth.4
Vitamin K
Vitamin K is another essential fat-soluble vitamin that also has two distinct forms. Vitamin K1 (phylloquinone) is mainly found in green leafy vegetables and some vegetable oils.2,7 It is the primary dietary source of vitamin K in the United States, whereas K2 (menaquinones [MKs]; e.g., MK-7 and MK-4) is found in butter, egg yolks, some cheeses, fermented dairy products, and is also produced by lactic acid bacteria in the intestine.2,7 Both vitamin K forms are deemed essential cofactors for the production of proteins that are involved in the homeostasis of calcium and blood coagulation.2
Functions of vitamin K
Vitamin K1: Transported to the liver and regulates cofactors that aid in coagulation of the blood.2
Vitamin K2: A cofactor for carboxylase activity, it facilitates the gamma-carboxylation of bone-specific proteins such as osteocalcin (OC) and matrix Gla (MGP).2 OC takes calcium from the blood and binds it to the bone matrix, which in turn helps increase bone formation.7 MGP inhibits vascular and soft tissue calcification.2
During vitamin K deficiency or insufficiency, osteocalcin and MGP remain uncarboxylated, which is associated with lower bone mineral density (BMD) and an increased risk of osteoporosis and cardiovascular disease.8
Common micronutrient shortfalls
According to nationally representative data, vitamins D and K represent common, significant nutrient gaps for the majority of Americans ≥ 2 years of age.9
Proposed synergy between vitamins D and K: bone
and cardiovascular health3
• Animal and human studies have demonstrated that vitamin D helps
stimulate the production of vitamin K-dependent proteins, OC and MGP,
which support bone mineralization and decrease vascular calcification.
• Long-term supplementation of vitamin D can lead to increased
production of vitamin K-dependent proteins. If the increased demand
is not adequately supported through diet or supplementation, the
proteins can remain uncarboxylated, which can lead to increased
vascular calcification and lower BMD.
• Excess supplemental calcium intake without the support of vitamins D
and K can lead to increased calcium deposits in the vascular tissue
instead of the bones.
Research
Bone health10
A randomized controlled trial involving 78 post-menopausal women aged 60-plus was conducted to assess the effects of vitamins D and K on BMD and undercarboxylated OC (UcOC) over a six-month period; 45 women completed the study.
The vitamin K group (n=40) received 15 mg of K2 TID after every meal,
400 IU calcitriol once daily, and 315 mg calcium carbonate BID. The
control group (n=38) received 400 IU calcitriol once daily and 315 mg calcium carbonate BID.
Results: There was a statistically significant (P=0.049) increase in lumbar spine (L3) BMD in the vitamin K group compared to the control group. In addition, compared to baseline, the vitamin K group significantly decreased UcOC concentration (P≤0.01). Osteocalcin also non-significantly increased in the vitamin K group. Some observational and animal studies also support these findings.3 There were some limitations to the study, which included the small number of participants, high dropout rate, and the absence of a separate comparator group that did not receive any supplementation.
Cardiovascular health11
In a study with 42 patients with chronic kidney disease (CKD) stages 3-5 (non-dialyzed), the researchers assessed the effect of vitamin K2 substitution on the progression of atherosclerosis and calcification for
nine months. The vitamins K+D group received 90 mcg of K2 with
10 mcg (400 IU) of vitamin D3. The vitamin D alone group received
400 IU of vitamin D3.
The common carotid intima-media thickness (CCA-IMT), coronary artery calcification score (CACS), uncarboxylated MGP, and osteocalcin levels were measured. They found the thickness of the CCA-IMT along with CACS were significantly lower in the vitamins K+D group compared to the vitamin D
only group. The uncarboxylated MGP and OC levels also significantly decreased in the K+D group.
Additional health benefits
Researchers are also studying the impact of joint supplementation of vitamins D and K on glucose metabolism and inflammation. These studies have found beneficial effects on markers of oxidative stress, upregulation of insulin receptor genes, and enhancement of β-cell proliferation.3


