
by Milene Brownlow, PhD
Overview
We are beginning to understand the wide-ranging impact of the coronavirus disease (COVID-19) on multiple facets of life. The outbreak that started late in 2019 was officially declared a pandemic by the World Health Organization and sent most of the world’s population into confinement. Beyond healthcare, this pandemic has drastically altered life as we know it.
Originally presented in the form of pneumonia of unknown etiology in Wuhan, China, it has since been determined that this respiratory infection is caused by a new strain of coronavirus (COV). The severe acute respiratory syndrome-related coronavirus (SARS-CoV-2) is an enveloped single-stranded RNA virus and infects neurological, respiratory, enteric, and hepatic systems. COVID-19 manifests with a wide clinical spectrum ranging from asymptomatic patients to septic shock and multiorgan dysfunction. The most common symptoms include fever, fatigue, dry cough, and diarrhea. Patients with mild illness, which represents a majority of the cases, may present with symptoms of upper respiratory tract viral infection that include: dry cough, mild fever, nasal congestion, sore throat, headache, muscle pain, and malaise.1
While social distancing remains the recommendation to minimize even greater dissemination of the virus, it does not come without deleterious health consequences. Social isolation or lack of social engagement results in psychological distress and a sense of loneliness, as recently published in JAMA.2 This feeling has, directly or indirectly, wide-ranging consequences for our psychological wellbeing as well as our physical health, even our longevity.
COVID-19 and the central nervous system
The role of the virus itself on the human central nervous system (CNS) is a less understood facet of COVID-19 that researchers are now uncovering. For some time, it was believed that the brain was immunoprotected from peripheral insult because of the existence of the blood-brain barrier (BBB). We now know that although the BBB plays a key role in separating the brain from immune cells in the bloodstream, it is a dynamic structure and is vulnerable to the peripheral environment. Chronic inflammatory conditions, infections, and other events affect its structure and permeability.3
As previously described here, neurological symptoms presented by COVID-19 patients such as confusion, insomnia, anxiety, and loss of sense of smell (anosmia) and taste (dysgeusia) may be explained by SARS-CoV-2 direct actions within the CNS. In fact, the American Academy of Otolaryngology-Head and Neck Surgery released a statement noting that anosmia and dysgeusia are symptoms associated with COVID-19 and may be used as a reporting tool for clinicians.4
In previous SARS-CoV infections, autopsy revealed the presence of the virus in the brain.5 Glial and neuronal cells express ACE2 receptors (shown in figure 1 below), making them a potential target of SARS-CoV-2, which might gain access to the brain via the bloodstream. Neurotropism may also occur via upper nasal route,6 enabling the virus to reach the brain. ACE2 and TMPRSS2, two proteins required for SARS-CoV-2 entry, are produced in cells in the nasal cavity that contribute to odor detection. This suggests a plausible route for SARS-CoV2 to infect the brain. Recent findings showed higher expression of these proteins in older mice than younger ones, likely explaining why older people are more susceptible to SARS-CoV-2.7 Another possibility is that systemic dysregulation caused by SARS-CoV-2 can result in respiratory failure and invasion of the brain stem respiratory centers via neuronal retrograde dissemination.8,9
Fig. 1
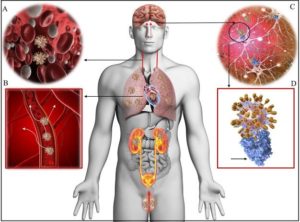
| Fig. 1: Tissue distribution of ACE2 receptors in humans. Viremia (A) disseminates the COVID-19 virus throughout the body via the bloodstream (B). Neurotropism may occur via circulation and/or an upper nasal trancribrial route that enables the COVID-19 to reach the brain (C) and bind and engage with the ACE2 receptors (D, blue). COVID-19 docks on the ACE2 via spike protein (D, golden spikes). Shown are lungs, heart, kidneys, intestines, brain, and testicles that are well-known to express ACE2 receptors and are possible targets of COVID-19. |
Roe K posed an interesting explanation as to why some viruses, such as SARS-CoV-2, selectively infect neurons.10 Activation of the innate immune system requires an antigen to be presented by another cell, such as dendritic cells, on a specific surface protein, known as major histocompatibility complex (MHC) or human-leukocyte-associated (HLA) antigens. Since neurons carry few antigen-presenting surface proteins required to activate immune T-cells, they cannot easily present viruses to cytotoxic CD8 T-cells,11 allowing viruses to evade attacks from the host immune system. As an example, herpesviruses also evade the host immune system by becoming latent with low replication while they infect neurons and can create lifelong infections that can be reactivated whenever the host immune system is weakened. Although some viral infections can be lifelong, there is no evidence that COVID-19 infections could be lifelong in survivors at this early stage.
Why is this important?
Regardless of how SARS-CoV-2 gains entry into the CNS, its presence in the brain has been confirmed by multiple findings.7,12 Treatments and therapies that minimize SARS-CoV-2 reaching the CNS may prove to be lifesaving by minimizing neurological damage and addressing cases where the occurrence of acute respiratory failures results in the need for ventilators in hospitalized patients.
Detailed neurological investigation and attempts to isolate SARS-CoV-2 from the CNS can clarify the role played by COVID-19 in the ongoing mortalities. Greater understanding of the neurotropic potential of the SARS-CoV-2 virus will allow for prioritization and personalization of treatment protocols based on disease severity. Future studies, as well as autopsy and pathology reports, will better arm the scientific community to fight against this pandemic.
Mental health burden of COVID-19
Since the beginning of time, humans have learned the advantage of social engagement and living as a group. From sharing knowledge and resources and relying on our community, we have all experienced the proverbial “it takes a village” feeling of accomplishing something with the help of others. In times of distress, human resilience depends on the richness and strength of social connections as well as active engagement in groups and communities.
Bzdok & Dunbar recently published a comprehensive review on the neurobiology of social isolation, highlighting the evidence for the many gains of social interaction and the impact of social deprivation.13 Of interest is the finding that loneliness and psychological distress directly impair the immune system, rendering us more susceptible to diseases and infections.14,15
Stress, whether positive or negative, is a natural process that allows our bodies to accommodate to changes. When stress becomes chronic, it exceeds buffering capacity and wreaks havoc on our bodies, affecting every biological system and pathway including hormones, sleep, metabolism, body composition, mood, cardiovascular health, and immune health. Higher levels of stress are to be expected when an already chronically stressed population goes through a worldwide pandemic.
One way to navigate this challenging time may be to channel stress into positive activity, for growth opportunities, for empathy, and for recognizing one another’s needs. Some suggested ways to mitigate possible negative effects of social distancing include:13
- Joining clubs that match people’s interests and lifestyle can help reduce both loneliness and psychological or psychiatric disorders.16
- Singing can have a dramatic and immediate effect on several brain areas associated with emotional behaviors. Its beneficial effects are modulated by endorphins, endocannabinoids, and dopamine and can be useful in the clinical management of psychiatric disorders.17
- Using digital and video-enabled means of communication can help people stay connected with family and friends. Being able to engage with social networks contributes to a mutual sense of belonging and support. Connecting visually seems to create an even more satisfying experience of digital social engagement.18
- Considering early and continuous psychiatric interventions for both healthcare workers and population in home quarantine can facilitate coping with the pandemic and economic turmoil and mitigate occurrence of chronic mental health disorders.
- Curbing exposure to social media and news. Sometimes constant exposure to conflicting and misleading information leads to higher levels of acute stress.
Why is this important?
While social isolation remains the most effective measure for containment of COVID-19, the long-term effects of this action, particularly on mental health, will not be fully appreciated for several years. The extent of fear, uncertainty, and frustration has real, pervasive, and diversified ramifications for each one of us. It may be that you are dealing with a sick loved one, caring for an at-risk individual, or shuffling working from home while overseeing your children’s homeschooling activities. No matter where you are during this time, your struggles and concerns are valid. Finding time for self-care becomes even more important when what is at stake includes the wellbeing of others. Self-care does not always come in the form of bubble baths, expensive spa treatments, or pushing yourself in the gym. Sometimes all you need is three minutes of sunlight and mindful breathing, or it could be starting a gratitude journal. It is even more important now to choose to focus on a sense of community. Bonding with your network of friends and family, encouraging others who may also be struggling, and amplifying the voices of those effecting positive change in the world are a great way to start.
Citations
- Hassan SA et al. Coronavirus (COVID-19): a review of clinical features, diagnosis, and treatment. Cureus. 2020;12(3):e7355.
- McGinty EE et al. Psychological distress and loneliness reported by US adults in 2018 and April 2020. JAMA. 2020. [Epub ahead of print].
- Haruwaka K et al. Dual microglia effects on blood brain barrier permeability induced by systemic inflammation. Nat Commun. 2019;10(1):5816.
- COVID-19 Anosmia Reporting Tool, American Academy of Otolaryngology-Head and Neck Surgery. https://www.entnet.org/content/coronavirus-disease-2019-resources. Accessed June 1, 2020.
- Netland J et al. Severe acute respiratory syndrome coronavirus infection causes neuronal death in the absence of encephalitis in mice transgenic for human ACE2. J Virol. 2008;82(15):7264-7275.
- Baig AM et al. Evidence of the COVID-19 virus targeting the CNS: tissue distribution, host-virus interaction, and proposed neurotropic mechanisms. ACS Chem Neurosci. 2020;11(7):995-998.
- Bilinska K et al. Expression of the SARS-CoV-2 entry proteins, ACE2 and TMPRSS2, in cells of the olfactory epithelium: identification of cell types and trends with age. ACS Chem Neurosci. 2020;11(11):1555-1562.
- Li Y et al. The neuroinvasive potential of SARS-CoV2 may play a role in the respiratory failure of COVID-19 patients. J Med Virol. 2020;92:552.
- Zhou L et al. SARS-CoV-2: underestimated damage to nervous system. Travel Med Infect Dis. 2020;24:101642.
- Roe K. Explanation for COVID-19 infection neurological damage and reactivations. Transbound Emerg Dis. 2020;00:1-2.
- Murphy K et al. Janeway’s Immunobiology: Immunobiology. 8th edition. New York:Garland Science;2012.
- Poyiadji N et al. COVID-19-associated acute hemorrhagic necrotizing encephalopathy: CT and MRI features. Radiology. 2020:201187. [Epub ahead of print].
- Bzdok D & Dunbar RIM. The neurobiology of social distance. Trends Cog Sci. 2020. [Epub ahead of print].
- Pressman SD et al. Loneliness, social network size, and immune response to influenza vaccination in college freshmen. Health Psychology. 2005;24(3):297-306.
- Cohen S et al. Psychological stress and susceptibility to the common cold. NEJM. 1991;325:606-612.
- Cruwys T et al. Social group memberships protect against future depression, alleviate depression symptoms and prevent depression relapse. Soc Sci Med. 2013;98:179-186.
- Boso M et al. Neurophysiology and neurobiology of the musical experience. Funct Neurol. 2006;21(4):187-191.
- Vlahovic TA et al. Effects of duration and laughter on subjective happiness within different modes of communication: happiness and mode of communication. JCMC. 2012;17(4):436-450.
Milene Brownlow, PhD is a Nutrition Scientist for the Cognitive Platform at Metagenics. She has earned her PhD from the University of South Florida, studying the role of diet-induced ketosis and calorie restriction on Alzheimer’s pathology. During her postdoctoral fellowship at the Air Force Research Laboratory she investigated nutritional approaches to optimizing brain health and cognitive performance. Dr. Brownlow has extensive experience in designing, managing and executing studies in behavioral neuroscience and has authored over 15 peer-reviewed publications. In her spare time, she enjoys spending time with her husband and their daughter, exploring the beautiful Pacific Northwest.






