by Michael Stanclift, ND
Even before the coronavirus (COVID-19) outbreak was declared a pandemic, we were having a tough season for respiratory illnesses. For example, in January both of my children developed severe respiratory infections requiring hospitalization. They weren’t diagnosed with COVID-19, but instead were sick from respiratory syncytial virus (RSV). The resources for their treatment are the same as for the current COVID-19 pandemic. As we were transferring my son to the pediatric intensive care unit (ICU), a nurse told me the respiratory illness season was just starting to ramp up and they were anticipating opening their 10-15 “overflow” beds in the next week. Coronavirus hadn’t yet taken off. Two months later, staring down a COVID-19 pandemic, 10-15 overflow beds at a hospital in a major metropolitan area (San Diego, California) seems woefully underprepared, if we don’t dramatically slow the rate of spread.
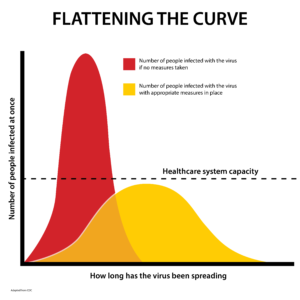
Flattening the curve
Figure 1
With over 191,000 confirmed COVID-19 cases, more than 7,800 deaths, and 154 countries/regions affected by the pandemic, the epidemiologists are really urging social distancing in an effort to “flatten the curve.”1 So what does that mean? Flattening the curve refers to slowing the spread of the virus, thereby reducing the numbers of active, severe illnesses at one time. If the coronavirus spreads through the population quickly, the small percentage of people who get severely ill will add up to large numbers, which will put a strain on our healthcare system. It’s easy to see how this number could exceed the dotted line (shown in red, Figure 1), overwhelming the healthcare system and leading to more deaths due to inadequate medical resources and care from the surge in infections occurring at one time. Below the dotted line patients have a fighting chance (shown in yellow, Figure 1) by slowing the transmission of the disease due to social distancing and implementing proper public health measures.
Therefore, by putting these measures in place, we can hopefully delay the spread of the virus, ultimately decreasing the number of new cases that are diagnosed at once and slowing down the number significantly. This allows the healthcare system to accommodate all the people who might become infected over time with the virus and provide proper care.
An article comparing the COVID-19 data available from Johns Hopkins University showed the United States’ rate of confirmed cases is trending similar to that of Italy, Iran, and South Korea—countries with some of the highest number of confirmed cases outside China.2
Let’s say a hospital has 10 doctors and 20 nurses it can call in for a shift. If they have 20 critically ill patients, each patient gets a dedicated nurse and half of one doctor’s attention during that shift. If 80 more severely ill people show up infected with the coronavirus the next day, the level of care lowers for all 100 patients. The hospital may not have enough beds/rooms/equipment to properly care for everyone who is sick. In my son’s case of RSV, we were transferred to the ICU so he could have closer monitoring and a high-tech ventilator that wasn’t available in the general respiratory ward of the hospital. A surging demand for ventilators would mean some of the critically ill patients who needed one wouldn’t have access, which is a very scary thought. We also must consider the health of the providers who are risking their lives caring for these patients. If a doctor or nurse caring for a sick patient gets infected with the coronavirus and has to take time off work, you can see how this further stresses the system. Another important thing to remember is that healthcare facilities for emergencies and the critically ill are often running at near maximum levels during this time of year due to other respiratory illnesses such as the flu and pneumonia.
How can you flatten the curve?
We know roughly 80 percent of COVID-19 illnesses will be mild, but each person who gets the coronavirus has the chance to spread it to others.3 You don’t want to be a spreader. The Centers for Disease Control (CDC) learned valuable lessons about flattening the curve from the 2009 influenza (H1N1) pandemic and published an update in 2017.4 Hand hygiene, social distancing, cancelling mass gatherings, and closing public spaces were found to be the most effective.4 Hand hygiene proved to have robust effects, with one study showing poor handwashing reduced infection rates by 74% and the best handwashing reduced rates by 97%. 4 A mandatory home quarantine prevented the H1N1 outbreak from being 5.6 times higher.4 An additional 1-2 days of paid sick leave reduced infections by 25.33-39.2%, respectively.4 School closures when a “low threshold” of H1N1 cases surfaced prevented over 830,000 infections.4
Another study in the report showed school closures reduced self-reported acute respiratory illnesses by 45%.4 Working from home “had a moderate effect,” reducing H1N1 transmission by 20-30%, and definitively had a delaying effect.4 Household quarantine was very effective for reducing total and peak cases.4 Surgical facemasks were effective if worn by sick patients: They reduced aerosolized viral shedding by 3.4-fold.4 Mask effects were less impressive when worn by healthy people, though in mass gatherings they reduced transmission by about 11% and are certainly an outward signal to others to keep their distance.4
One study in a dorm setting showed a 75% reduction, though many institutions have already gone the route of sending their students home.4 If you must go out, keep six feet away from people and avoid gatherings of 10 people or more.5 By following these evidence-based recommendations, you can dramatically reduce exposure to nearly all infectious illnesses, which decreases overall healthcare demands. If you develop respiratory symptoms, call your healthcare provider. Ask for the best course of action before showing up and potentially exposing people who may be at risk and visiting for another reason.
You’ll save lives by slowing the spread and flattening the curve of COVID-19.
Citations
- World Health Organization. Coronavirus disease 2019 (COVID-19) Situation Report-58. https://www.who.int/docs/default-source/coronaviruse/situation-reports/20200318-sitrep-58-covid-19.pdf?sfvrsn=20876712_2. Accessed March 18, 2020.
- Scott D et al. How the US stacks up to other countries in confirmed coronavirus cases. Vox website. https://www.vox.com/policy-and-politics/2020/3/13/21178289/confirmed-coronavirus-cases-us-countries-italy-iran-singapore-hong-kong. Updated March 16, 2020. Accessed March 17, 2020.
- World Health Organization. Coronavirus disease 2019 (COVID-19) Situation Report-41. https://www.who.int/docs/default-source/coronaviruse/situation-reports/20200301-sitrep-41-covid-19.pdf?sfvrsn=6768306d_2. Updated March 1, 2020. Accessed March 16, 2020.
- Qualls N et al. Community mitigation guidelines to prevent pandemic influenza – United States, 2017. MMWR Recomm Rep. 2017;66(1):1-34.
- Interim Guidance for Coronavirus Disease 2019. Centers for Disease Control website. https://www.cdc.gov/coronavirus/2019-ncov/community/large-events/mass-gatherings-ready-for-covid-19.html. Updated March 15, 2020. Accessed March 16, 2020.
Michael Stanclift, ND is a naturopathic doctor and senior medical writer at Metagenics. He graduated from Bastyr University’s school of naturopathic medicine and practiced in Edinburgh, Scotland, and Southern California. He enjoys educating other healthcare providers and impacting the lives of their many patients. When he’s not working, he spends his hours with his wife and two children.